
INTRODUCTION
Access to affordable healthcare continues to be a challenge for most Nigerians due to high levels of poverty and significant reliance on out of pocket payments. Health Insurance coverage throughout the country has barely scratched the surface relative to the country's rapidly growing population.
According to statistics from the Nigerian Economic Recovery & Growth Plan 2017-2020, the average life expectancy in Nigeria is 52 years, significantly lower than that of its peer African countries, for example Ghana (61 years) and South Africa (57 years). On under-five child mortality, there are 89 deaths per 1,000 live births, a level far above the target of 64 deaths per 1,000 live births set in the UN Sustainable Development Goals (SDGs).
The development of the Nigerian healthcare system has been hindered by several notable challenges, including limited public funding, a high communicable diseases burden, rising incidence of non-communicable diseases, elevated rates of infant and maternal mortality. The World Health Organisation (WHO) notes that there is high reliance on out-of-pocket (OOP) health payments as a means of financing the health care system in Nigeria and that this has continued for many years in spite of a consensus to move closer to Universal Health Coverage (UHC) and sustain it when achieved.
The National Health Act (NHA) of 2014 established a legal framework for the development, regulation and management of a national health system and set standards for service provision. The latest version of the National Health Policy (NHP), which was approved in February 2017, dovetails with the NHA in an effort to attain the UN’s SDG 3, particularly on Universal Healthcare Coverage. The NHP establishes a framework for harnessing health development resources, with a focus on primary care networks, and seeks to increase the efficiency and affordability of service delivery. It contends to do so via 10 “policy thrusts” in areas as varied and connected as governance, financing, medicines and vaccines, infrastructure, data systems, research and development, Public-Private Partnerships (PPP) and community participation.
According to Fitch Solutions, Healthcare expenditure in Nigeria is predicted to reach NGN 5,762.061 billion by 2021 up from an estimated NGN 5,318.061 billion in 2020. By 2021, healthcare spending is estimated to make up 2.94% of the country’s GDP, which is miles off the WHO recommendation that at least 5% of GNP is spent on health. While the government is expected to spend NGN 1,477.77 billion by 2021, the private sector will spend NGN 4,284.469 billion in the same period.
In response to this, in the last 10 years of its operations, the WBFA has provided financing and healthcare provision through the Indigent Medical Fund, The Twins and Multiple Birth Program, and the Positive Lifeline Program. Since 2015, we have reviewed our operations to ensure our impact continues to be effective and far-reaching.
Considering that approximately 53.47% of Nigerians live below $1.90 a day, subsidised health insurance can be the difference between life and death for a number of families. Out-of-pocket financing at the point of service in hospitals can cripple families financially for years, resulting in further economic vulnerability and limited access to regular primary healthcare, setting off a cycle of poverty and poor health for generations.
For this reason, WBFA decided to transform and merge our existing health financing schemes to initiate the Alaafia Universal Health Coverage Fund (AUHCF) in partnership with Hygeia Community Health Care (HCHC) - a local health insurance provider -, PharmAccess Foundation and the Kwara State Government. Through the AUHCF, we funded the insurance premiums of 5000 people each year.
The AUHCF served enrolees with an estimated percentage representation at the following levels: infants 35%, under-five children 30%, pregnant women 13%, persons living with HIV/AIDS and/or disability 12%, the elderly 3%, girls (aged 6-13 years) 7%. This was the planned spread across specific low-income communities in Kwara State, north-central Nigeria, in order to ensure that healthcare got to more people who lack the financial and geographical access to healthcare.
WBFA is continuously seeking ways to improve and expand AUHCF, in order to bring the strategy of Universal Health Coverage (UHC), as championed by the World Health Organization and the World Bank, to those in need.
Research has shown that investing in reproductive, maternal, newborn, child and adolescent health (RMNCAH) could yield up to nine times its value in economic and social benefits, and healthy home practices and community-based care could save over 90 000 babies a year.
Primary healthcare over emergency care not only avoids high out-of-pocket spending, but also educates mothers about their health and the health of their children. This will empower women to make informed decisions about their care, in partnership with their healthcare provider, setting the foundation for respectful maternity care and improved long-term relationships with healthcare professionals. Establishing a relationship of respect and trust with healthcare professionals during adolescence will also encourage young girls to overcome cultural stigmas regarding their reproductive health, and engage in health-seeking behaviour throughout their lives for the benefit of their entire families.
OBJECTIVES
WBFA strongly believes in and actively cultivates strategic partnerships and alliances to deliver on her mission to empower communities, families and healthcare workers with the right skills and information and maximise their access to life-saving commodities, facilities, and care.
Our vision for AUHCF includes:
- Advocacy and policy to ensure Universal Health Coverage.
- Access to Healthcare
- Promote financial inclusion.
- Reduce mortality rates through subsidized Health Insurance.
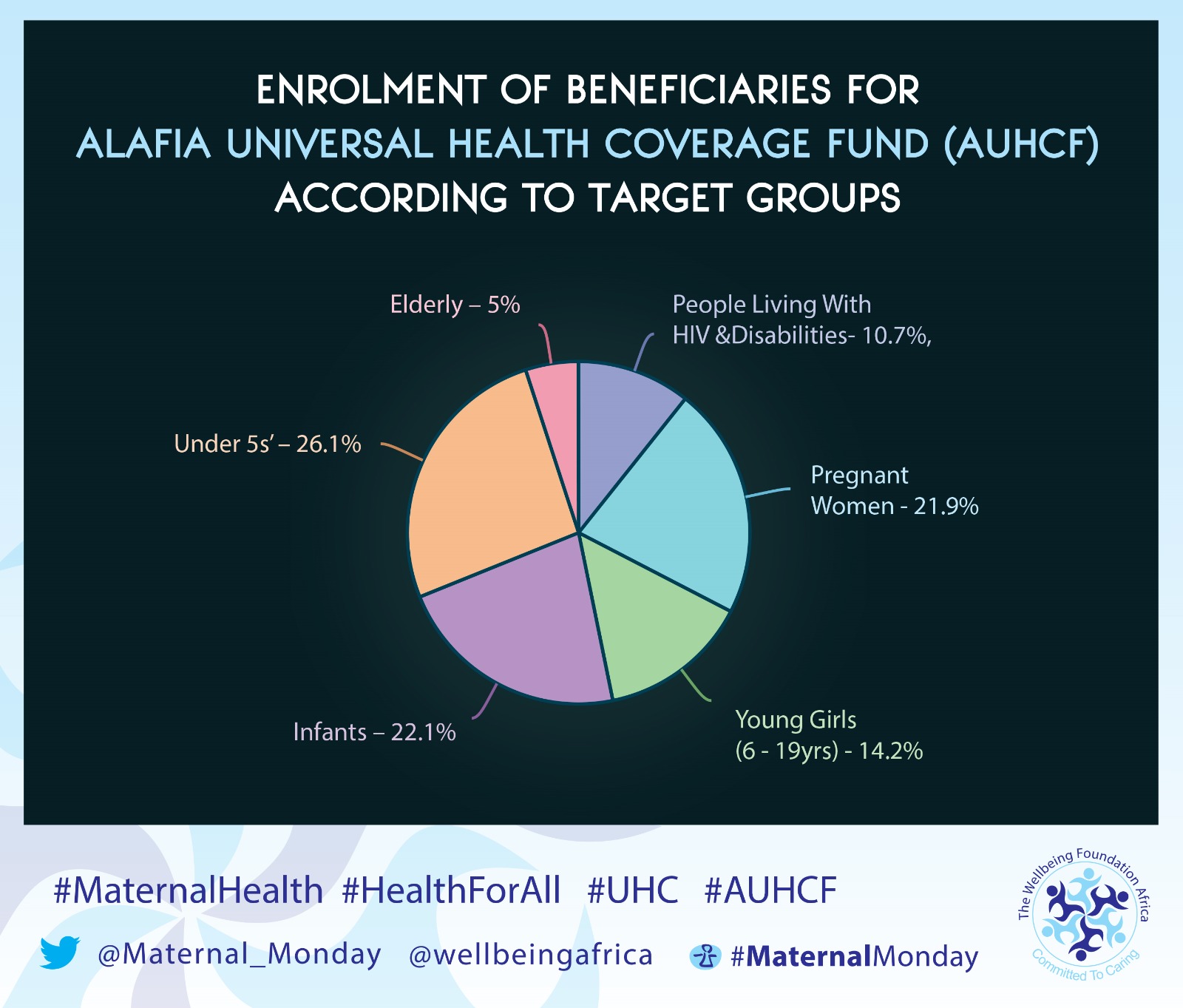
OUR RESULTS
- A total of three thousand nine hundred and seventy-one (3,971) enrolees were registered on the scheme between March 2015 and December 2015 (ten months).
- The total number of lives registered was 96% of the set target (4,128) during the same period.
- 864 pregnant women making up 23% of the total number were registered under the scheme.
- 876 infants making up 23% were captured by the scheme
- 1,039 under five children, 27% of the total number, excluding children noted in the infant category, were registered under the AUHCF.
- Young girls (6-19 years) were 562, 12% of the total number of enrolees.
- The elderly, 201, accounting for 6% of the total number of enrolees.
- 424 (9%) Persons Living with HIV (PLHIV) and persons living with disabilities were also beneficiaries of the scheme.
- The beneficiaries had access to comprehensive maternal services and child healthcare services on the AUHCF.
- The programme covered 24 healthcare facilities across 9 out of the 16 Local Government Areas in Kwara State.
- The LGAs covered were Asa, Edu, Oyuin, Kaiama, Oke Ero, Ekiti, isin, Baruten and Moro in Kwara State.
