International Universal Health Coverage Day: The Wellbeing Foundation Africa’s Commitment to a Whole-System Approach to Health for All
Today, as we mark International Universal Health Coverage (UHC) Day, I am encouraged by the growing momentum behind the belief that every single person should have access to the care they need when they need it, and that no one should be forced to suffer financial hardship or forgo treatment they cannot afford. The Wellbeing Foundation has committed to employing a whole system approach for health for all with ten essential features, centring on the provision of quality primary health care for all, with a focus on women, infants, and children. It has been three months since the High-Level Meeting (UN HLM) on Universal Health Coverage at the 74th UN General Assembly, in which leaders around the world recommitted to their promise of health for all. At the heart of this progress is the understanding that quality maternal care should be at the centre of our drive to achieve universal health coverage. I believe that it is critical that next year has been identified as the World Health Organization (WHO) Year of The Nurse and The Midwife. The year, which fittingly marks the 200th anniversary of the birth of Florence Nightingale, presents us with a unique opportunity to consider the role of gender parity and equality in health coverage and health provision.
In March 2019, the WHO, the Global Health Workforce Network, and Women in Global Health produced a report on Global Health and Social Workforce entitled “Delivered by Women, Led by Men: A Gender and Equity Analysis of the Global Health and Social Workforce.” Strikingly, the report found that ‘women deliver global health and men lead it’. The report highlighted that women comprise 70% of the global health workforce, but only 25% hold senior roles, while women face gender discrimination, barriers, and inequalities not faced by their male colleagues at work. Gender inequality within the sector is not only unacceptable, but it ultimately weakens the quality of healthcare that we are able to provide.

Nurses and midwives represent half of the professional health workforce and are overwhelming, although not exclusively, women. They play a critical role not only in delivering healthcare to millions of people in every country, but they are key to transforming health policies, disease prevention, emergency care, and supporting the families of patients. They are necessary partners supporting the health and wellbeing of the communities they serve in a multitude of ways that include health care delivery, education, and counselling. If we are to build universal health coverage that is of quality and value, it is essential that we ensure that frontline workers in maternal care have not just a have a seat at the table but sit at the head.
As nations develop UHC frameworks, I am encouraged to see a groundswell in the number of individuals and organisations advocating for sexual and reproductive health and rights (SRHR) and prioritising the needs and rights of women and girls. SRHR means liberating women and girls with access to family planning and empowering them with the information and confidence to make informed decisions about their lives. Strong SRHR frameworks include education, awareness, and choice: the choice to have children in clean and safe conditions. The choice to space children, so that resources can be distributed to maximise the opportunities of each child. The choice to be properly informed and empowered in the decision-making process that surrounds these issues is important for the young. Effective SRHR may prioritise women and girls, but it also cannot afford to exclude men and boys; these are issues that affect everyone.

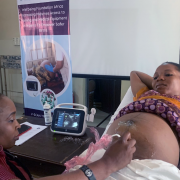
A MamaCare+N midwife delivering frontline care to a MamaCare mother and her family.
In 2013, at the World Health Assembly, then-President of the World Bank Group, Dr Jim Yong Kim, asserted that “we must be the generation that delivers universal health coverage.” I couldn't agree more: now is the time to get this right. In alignment with World Health Organization recommendations, the Wellbeing Foundation Africa’s whole system approach to UHC is comprised of ten essential components: 1) Pregnant women should receive the right care, at the right time; 2) Newborns should receive essential care immediately after birth; 3) Small and sick babies should be well cared for in a facility; 4) All women and newborns must receive care that prevents hospital-acquired infections; 5) Health facilities must have an appropriate physical environment; 6) Communication with women and their families must be effective and respond to their needs; 7) Women and newborns who need referrals can obtain them without delay; 8) No woman should be subjected to harmful practices during labour, childbirth, and the early postnatal period; 9) Health facilities need well-trained and motivated staff consistently available to provide care; 10) Every woman and newborn should have a complete, accurate, and standardized medical record. Each of our flagship programmes and initiatives; our Emergency Obstetric and Newborn Care programme, our Water, Sanitation, and Hygiene programme, our Personal Healthcare Record Book initiative, our Alive and Thrive programme, and our MamaCare/MamaCare+N programme are tailored to meet these priorities.
This year, leaders made progress by affirming UHC as a key strategic interest. But millions of lives hang in the balance of this essential promise, a promise on which we must deliver. The WHO cites that today approximately half of the world’s population live without full coverage of fundamental health services while an estimated 100 million people are being forced into extreme poverty due to health care expenses. The equivalent of one in ten people is spending over 10% of their household budget on critical health care costs. We know that there is a myriad of ways that health will impact the achievement of sustainable development, including, but not limited to the health-specific objectives. How can we solve poverty if people are forced into bankruptcy themselves to pay for treatment? We will only meet all of the SDGs by 2030 if everybody is able to access affordable, safe, respectful, and quality healthcare.
Today I call on all health partners and stakeholders to urge our leaders to deliver on their promise of UHC. I wholeheartedly believe that we must collectively champion UHC frameworks that are grounded in equality and inclusion and take into consideration not only the unique experiences of women in the health workforce, but that centre on SRHR policies that prioritise women and girls.
Share this Article

Toyin Ojora Saraki
Toyin Saraki is Founder-President of the Wellbeing Foundation Africa (WBF Africa), a pan-African maternal health and wellbeing charity. WBF Africa has become one of the most influential and active organisations in the area of maternal, newborn and child health (MNCH), working across sectors to deliver innovative solutions such as its flagship WBFA IMNCH Personal Health Record© and the MamaKit. WBF Africa goes beyond aid; it is dedicated to advocacy and the formation of best practices in health, education, women’s empowerment and social welfare. A qualified barrister, Toyin Saraki built a successful private sector career before dedicating the last 21 years to philanthropy.
Read More